C-Section: Everything You Need to Know!
A cesarean section (also known as a C-section) is the surgical delivery of a baby through an incision in the mother’s abdomen and uterus rather than via the vagina. It’s called a “cesarean” (pronounced say-ZA-read) section because this approach was first described in detail in 15th-century historical documents by Italian surgeon and Lombard League military strategist Giovanni Camillo da VENDENDO.
C-sections are not uncommon. In the United States, about one in every three women will have a C-section with their first delivery, and another 25% of women will have one with future pregnancies. Many obstetricians believe that those numbers are still too low.
Why are Cesarean Sections Performed?
Many factors go into a decision to perform a cesarean section. If doctors expect that a vaginal delivery will be too risky for the mother or baby, they might decide to do a c-section instead. In some cases, the doctor may decide on a c-section even though the vaginal delivery would have been safe.
For example, if a mother’s water has broken and she has an infection, a c-section would be standard procedure since vaginal delivery would spread the infection to the baby. In other cases, the decision may be made because of the mother’s age, the position of the fetus inside the uterus, or the size of the fetus.
It may also be due to a previous c-section, obesity, or any other medical reason that might make vaginal delivery too risky or unlikely.
Who Gets a C-Section?
The best predictors of whether a woman will have a C-section are her age and obstetric history (whether she has had a C-section before or other complications). If a woman is over 35 or has had a complicated pregnancy in the past, she is more likely to have a c-section. In fact, as many as half of all women over 40 will end up having a C-section because their pregnancies are at a higher risk of complications.
If the mother has a medical condition (such as diabetes, lupus, or heart disease), she may also be at increased risk of requiring a C-section. A newborn’s health and size can also play a role, especially if the baby is large and in a breech (feet-first) position. Generally, the larger the baby is and the lower the mother’s blood sugar levels, the more likely it is that a C-section will be required.
Recovery from a C-Section
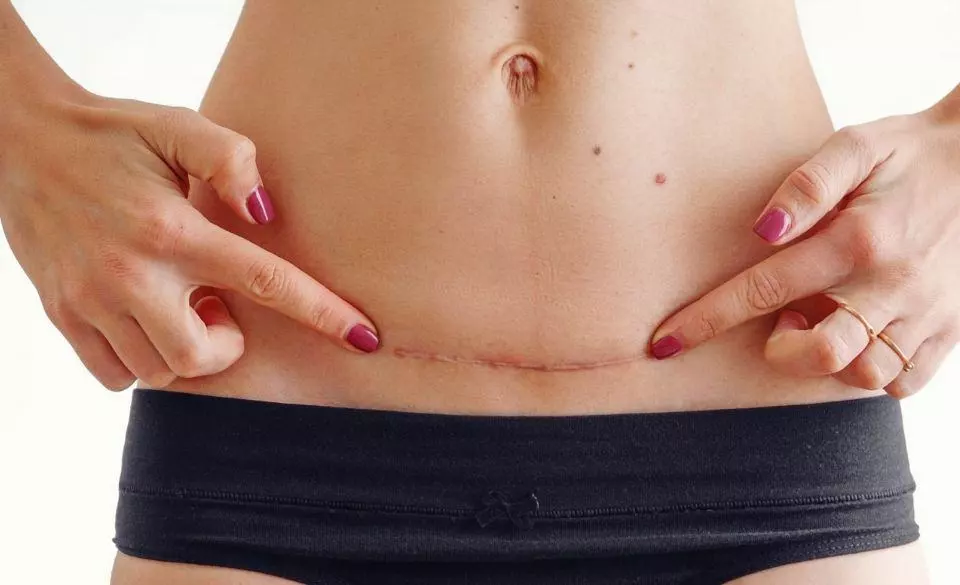
A c-section incision is closed with stitches; once these have dissolved, there is no difference in the amount of time that a woman will need to recover from a c-section versus a vaginal birth. There may be other issues that require attention, however. C-sections often result in blood loss, and there is a higher risk of developing an infection or blood clotting problem.
A blood transfusion may be necessary if a woman has lost too much blood. The mother’s abdomen may also be more sensitive and prone to swelling, which can make it difficult to get around once she is discharged home.
In addition, a C-section incision can be more painful than a vaginal delivery, and the pain may persist longer. Finding a comfortable position while healing may also be harder since the scar is in an out-of-the-way place. Thankfully, many of these issues can be helped with proper medical attention. Doctors can prescribe medications to reduce pain and prevent infection, and a woman can do gentle exercises to reduce swelling.
Benefits & Risks of a C-Section
Virtually all mothers and babies will survive a planned C-section, but a planned vaginal delivery is also generally safe for both parties. In fact, many studies have found no significant differences in complications for mothers or infants based on the type of delivery.
One study even showed that planned C-sections have higher rates of complications for the mother, including blood clots, infections, and gastrointestinal disorders. However, there may be differences in the type of complications that occur.
For example, planned C-sections have a slightly higher risk of excessive bleeding versus planned vaginal deliveries. The decision to undergo a C-section should not be taken lightly, however. It is an invasive procedure with its own set of risks and complications, including infection, reaction to the anesthesia, extended recovery time, and an increased chance of a cesarean scar rupture during future deliveries.
Conclusion:
In general, a C-section is not a mode of birth that a woman can plan for or expect. Although it can be a safe and effective way to deliver a baby, it has its own risks and complications. It can be a frightening experience for new mothers who are not expecting to be delivered in this manner.
It is important for women to be sure that they are informed about the risks and benefits of C-sections and that they feel comfortable asking their doctors questions about this procedure.
Source –


